|
Last week, we learned that we have special receptors, called nociceptors, on the ends of our nerves that send pain signals through the nerves to the spinal cord to the brain. These signals warn us about temperature, injury, irritation, or potential injury. Today, we'll cover neuropathic pain - what it is and how it's treated.
Neuropathic pain comes directly from the nerves, not the nociceptors. Nerves from the peripheral nervous system or the central nervous system may be affected. One or more nerves may be injured, damaged, irritated, 'pinched' (compressed from inflammation, disc material, or other matter), or functioning improperly. If you herniate a disc in your spine, some of the jelly-like material (the nucleus pulposus) may squirt into and block the passage designed for the nerves that are exiting from the spinal cord and going into an arm or leg. When that happens, the nucleus pulposus may touch or compress the nerve bundle which can cause severe neuropathic pain. Excessive repetitive motion, or a disease like Diabetes, can cause damage to nerves so that they function improperly and cause pain that may tingle and burn (called peripheral neuropathy). Phantom limb pain also falls in the category of neuropathic pain. Neuropathic pain is more likely to be chronic and can be more difficult to treat. While OTC analgesics can help with nociceptive pain, they do very little (if anything) to relieve neuropathic pain. Finding and resolving the cause of such pain is the first step in treating it. However, if the cause is known but cannot be remedied, other steps become necessary. Stronger medications, like opioids will probably be prescribed, but may or may not help. Using devices like TENS Units or Spinal Cord Stimulators may help block neuropathic pain signals from reaching the brain. For the naturalist, aromatherapy and herbal remedies may be the answer. What I find in my own case is that a combination of therapies is most effective. I have both nociceptive pain from osteoarthritis (all joints), and neuropathic pain from multiple bulging, herniated, degenerative, and fused discs. Opioids are not an option for me because they make me violently ill. Herbs and essential oils do help, and in combination with spinal cord stimulators, I get enormous relief. Because the stimulators interrupt the pain signals, they provide significant relief for both types of pain. The most important thing for those of you who suffer with neuropathic pain is to work with your health care practitioner to find the best therapies for your individual case. Sources: 1. Dresden, Danielle, Nociceptive and neuropathic pain: What are they?, Medical News Today, Last reviewed November 2, 2017 https://www.medicalnewstoday.com/articles/319895.php Accessed June 19 - 25, 2019 2. Smith, Yolanda, What is the Difference Between Nociceptive and Neuropathic Pain? , News-Medical Life Sciences, Last updated August 23, 2018, https://www.news-medical.net/health/What-is-the-Difference-Between-Nociceptive-and-Neuropathic-Pain.aspx Accessed June 19 - 25, 2019 3. Booth, Keley John, MD, Understanding Nociceptive and Neuropathic Pain, Pain-Health, Last updated September 27, 2018, https://www.pain-health.com/conditions/chronic-pain/understanding-nociceptive-and-neuropathic-pain Accessed June 19 - 25, 2019 4. Webberley, Helen, Dr., What is peripheral neuropathy?, Medical News Today, Last updated November 27, 2017 https://www.medicalnewstoday.com/articles/147963.php Accessed June 19 - 25, 2019 We've discussed pain from a personal perspective over the last two weeks. For these next two blogs, we'll explore what scientists have learned about pain. This week, the focus will be on nociceptive pain, and next week it will be about neuropathic pain.
In looking at the definition of pain, I find articles that define it as physical or mental discomfort caused by stimulus to nerve endings that signal harm or possible harm being done to the body. More simply stated, some thing (i.e. heat, pressure, sharp object, infection) triggers your nerves to send an "It hurts!" message to the brain. The Mayo Clinic explains the pain process clearly. We have a central nervous system (CNS) which is made up of our brain and spinal cord. The rest of the nerves in our bodies are called the peripheral nerves and are part of the peripheral nervous system (PNS). On the ends of the peripheral nerves are receptors called 'nociceptors'. Nociceptors are found throughout our bodies -- in joints, skin, bones, soft tissue (muscles, cartilage, ligaments, etc), and around internal organs. They sense stimuli that may cause harm and send electrical impulses through the peripheral nerves to the spinal cord. If you develop an infection in your appendix you feel visceral nociceptive pain. Visceral refers to pain in the abdomen or organs. If you stub your toe or twist your ankle, you feel somatic nociceptive pain, Somatic refers to pain everywhere else. From the spinal cord, the 'messages' are prioritized (or triaged) before being sent to the brain. The signal(s) sent in the case of a minor bump may be sent to the brain more slowly than signal(s) from a smashed finger. In the case of a minor bump, the brain's response may only focus on sending messages to your immune system to start the healing process. (Did you ever see a bruise on your leg and have no idea how it got there? You may not have noticed the bump, but your brain signaled your immune system to repair the minor damage.) If your finger is smashed in a door, your brain will immediately signal your body to remove your finger from the door and to start the healing process. The signals are sent so fast that your reaction is considered to be a reflex -- your brain uses pain to tell you to remove the damaging condition. In all of these situation, nociceptors initiate chemical and electrical messengers which travel through the peripheral nerves to your spinal cord, and your spinal cord relays those messages to your brain. This seems relatively straightforward, but there's more to pain. Scientists are finally trying to learn exactly how pain signaling works in our bodies, and they have made some interesting discoveries and hypotheses. First, pain physically changes brain and spinal cord cells and creates 'pain memory'. It's believed that this pain memory may play a role in chronic pain that occurs even after an injury has healed. Second, genetics may affect how a person responds to pain stimuli - whether that person is very sensitive to pain or has a high tolerance for it. When someone is very sensitive to pain, it's because the signaling is faster, and possibly stronger, in their PNS and CNS. Third, there is a gene called COMT which has different activity rates in different people. Those with a very active COMT may tolerate much higher levels of pain. So what does this mean for those with chronic nociceptive pain? One belief is that those with higher sensitivity to acute pain have a higher likelihood of eventually experiencing chronic pain. I'm not convinced that this is the case because I know many people who have a very high pain tolerance who live with severe chronic pain. I expect more studies need to be done in this area. Pain is considered chronic when it lasts beyond the time when an injury has healed. It's possible that the initial injury caused the nerves to become extra sensitive so that pain is felt more easily in that area. Again, I am left with questions. Given that it takes about 42 weeks (that's nearly a full year) for a damaged ligament to heal, is it really 'pain memory' causing us to imagine that there is still pain? Is it possible that chronic nociceptive pain is caused by micro damage that takes much longer (i.e. years) to heal? Scientists don't have answers to these questions yet. Perhaps one day they will. Sources: 1. Mayo Clinic, Understanding Pain, June 26, 2016 https://www.mayoclinic.org/understanding-pain/art-20208632 Accessed June 10 - 18, 2019 2. Felman, Adam, What is pain and how do you treat it?, Medical News Today, Last updated July 27, 2017, https://www.medicalnewstoday.com/articles/145750.php, Accessed June 10 - 18, 2019 3. Weir, Kirsten, Owww! The science of pain, Science News for Students, June 25, 2014 https://www.sciencenewsforstudents.org/article/owww-science-pain, Accessed June 14 - 18, 2019 4. Stace, Richmond, What is Pain? A Modern Scientific Perspective, Ezine Articles. April 9, 2010, https://ezinearticles.com/?What-is-Pain?-A-Modern-Scientific-Perspective&id=4074205, Accessed June 14 - 18, 2019 Last week, we discussed pain levels from a personal perspective. This week, we'll investigate how to describe different kinds of pain - again from a personal perspective.
When you go to the doctor's office, (s)he may give you a chart or ask you to describe your pain. Many of those charts will contain the following list (or something very similar): ache, sharp, burning, stabbing, throbbing. These adjectives are usually enough for those who occasionally experience pain, but if you live with chronic pain, describing that pain can be more complicated. It's okay (and probably more helpful) to give a detailed description of your pain to your doctor. For example, when you tear soft tissue, like cartilage or a ligament, initially, it's a severe, intense sensation like scissors were used to cut something inside your body. (It's a feeling you never forget and will recognize if/when it happens again.) Over a few minutes, the severity of the pain diminishes to a strong feeling of pressure. Depending on where the tear occurs, mobility of a limb may be partially or totally impaired, but by the time you get to a doctor, you may only feel a mild ache (or no pain) at rest, and moderate to severe heaviness, pressure, and/or tearing pain with motion or weight bearing. Nerve pain, like sciatica, can feel like a blowtorch is shooting down your back into your butt and/or leg(s). That pain may start suddenly or gradually and may be fleeting or last for hours/days/weeks/months. Other nerve pain may feel like you're being pricked with a thousand pins or like you're being seared with an iron bar fresh out of a forge. Bursitis may feel like a foam-filled balloon is stuck in your joint and is trying to explode - the pressure moves from the center outward. Blocked Eustachian tubes or an ear infection may have a similar sensation. Breaking a bone feels like a combination of an initial snap followed by the sensation of a molten iron poker being stuck in the bone. Unlike a soft-tissue tear, it takes days for this intense pain to subside. These are just a few examples from my perspective. You may have different descriptions for similar conditions -- it's important to give your doctor as accurate a picture of your pain as possible. For more serious pain, that description should go beyond ache, sharp, burning, stabbing, throbbing. Next week's blog will delve into the scientific perspective of pain - its purpose, how the body knows to "feel pain", and how the pain signals are sent through the body. Most of us have experienced physical pain at some point in our lives. Sometimes, it's minor, other times it's major. Doctors have a 1 - 10 scale they ask us to use to quantify our pain. For some, pain is something that occurs occasionally; for others, it's chronic - daily, perhaps 24/7. Today's blog will talk about pain from a personal perspective.
Doctors say level 1 is no pain. A mosquito bite itches. A paper cut stings. These are examples of mild/minor pain -- probably a level 2 - 4 on the doctor's scale. Sore muscles, bumps, and bruises may cause moderate pain - levels 5 - 7. Sprains, ligament tears, some migraines are examples of severe pain -- levels 8 - 10. A broken bone would be an example of level 10 pain -- a level that physicians consider to be the most severe. This scale works quite well for those who sometimes experience pain, but there is pain that goes beyond these levels. Sciatica, neuropathy, extreme migraines are a few examples of excruciating pain - what I call levels 11 - 13. Level 11 is stronger pain than a broken bone. It reduces the ability to concentrate and to function, and leaves the person exhausted, but unable to sleep for more than an hour or two at a time. Level 12 further reduces concentration, the ability to function, and memory. The person might be able to get 1/2 to 1 hour of sleep at a time. At this level, when going to bed at night, the person thinks 'It's okay if I die before I wake up because I'll be out of pain.' (I know, this is unimaginable to many, but those who live with this level of pain understand exactly what I'm saying.) Level 13 is pain so intense that the person is no longer able to think or function - (s)he is only able to moan, groan, and cry. What do we do about pain? For mild to moderate pain, we may just put up with it, ignore it, or take acetaminophen or ibuprofen. For severe pain, most people will take an analgesic, OTC medication, or get a stronger, prescription medication. Excruciating pain needs greater intervention. It may need stronger medications, bracing, or even surgery. Severe and excruciating pain levels definitely require a visit to the doctor for diagnosis and treatment plans. But, what if pain meds make you so sick you can't take them? There are many of us who experience that. Fortunately, there are alternatives for those of us who are adversely affected by pain meds -- and for those who prefer to use natural methods as much as possible. What are those alternatives? Alternatives include physical therapy, chiropractic care, acupuncture, use of herbs (TCM, Ayurveda, Western Herbalism), and using essential oils and fixed/carrier oils. If you are looking for more natural methods of soothing your pain, check with an expert in one (or more) of these therapies. You can also start your own journey studying these fields! I remember drinking whole milk and using real butter when I was young. While Mom rarely fried our food, she did use natural butter and oils. Sometime in the 70's, we started hearing on the media that the 'experts' decided that whole milk, lard, and real butter were bad for the heart, and that hydrogenated fats like margarine would make us all healthier. In the 90's, suddenly all fats were bad for us -- coconut oil became enemy # 1 and movie theaters stopped using it to make their popcorn. In the last 10 years or so, milk has become the new enemy. To this day, even our doctors will tell us to cut out the fats from our diets and stop drinking real milk. Just last week, my doctor told me to switch to soy or almond "milk". Sadly, those recommendations were, and are, seriously flawed and have caused a great many more health issues for millions of people. Many people and many doctors are unaware that scientists now recognize that we need saturated, unsaturated, and polyunsaturated fats in our diets. Today, we'll learn about the two Essential Fatty Acids (EFAs) found in these fats that we MUST consume because our bodies don't make them and discuss the importance of their Omega classifications.
The two Essential Fatty Acids are Linoleic Acid (LA) and Alpha-Linolenic Acid (referred to as ALA or LNA). They are called essential because we have to ingest them in order to survive. The cells in our bodies consist of 60% fat for brain cells and 50% fat for all other cells. So fats are some of the nutrients needed to keep every cell healthy. Other Fatty Acids can be made by our bodies when we eat the proper foods, but LA and LNA are not made by our bodies, and must be eaten to help produce metabolic compounds that are required to get nutrients to all of our cells. These two EFAs are polyunsaturated, have polar opposite functions in the body, and need to be balanced! Linoleic Acid is found in meats, seeds, nuts, and vegetable oils. Grape-seed, Corn, Evening Primrose, Sunflower, Safflower, and Soybean oils are all high in LA. In the oils, LA is more stable (takes longer before spoiling) than LNA, so companies making processed foods (like chips) prefer to use oils with a higher LA content. This is important because LA is a pro-inflammatory, Omega 6 fatty acid. If you read my last several blogs, you know that we need inflammation - it's the way the body protects and heals itself, and that the inflammation process includes swelling and resolution of swelling. Internally, Linoleic Acid promotes the inflammation portion of the inflammatory process -- it supports the metabolic processes that cause inflammation in response to a threat, injury, or invasion. Topically, LA supports the barrier function of our skin -- it keeps harmful invaders out. Yet, it also supports the passage function -- it absorbs easily and brings nutrients and moisture deep into the layers of the skin. LA helps keep our skin healthy and moisturized. Alpha-Linolenic Acid (ALA)(LNA) is found in sardines, mackerel, fish oils, wild salmon, navy beans, hemp seeds, edamame, flax seeds, whole wheat, walnuts, avocados, chia seeds, perilla, oatmeal, etc. Oils high in LNA include Flax, Chia Seed, Kiwi, Perilla, Sea Buckthorn, Sacha inchi, Camelina, Rosehip Seed, Kukui Nut, Blueberry, Cranberry, Red Raspberry, Hemp Seed, Blackberry, and Walnut. LNA is not as stable as LA, so products made with a high percentage of LNA will spoil more quickly. LNA is an anti-inflammatory, Omega 3 Fatty Acid. It promotes the reduction of inflammation by supporting the metabolic processes that resolve inflammation once the affected body part is healed. Internally, LNA supports circulation, heart health, eye health, and blood pressure, and is useful in the prevention of obesity, arterial, rheumatic, and autoimmune illnesses. In infants and children, it helps with brain and eye development. Current studies are showing the possibility that when properly combined with Linoleic Acid, LNA could lower the incidence of respiratory infections in children. Topically, LNA is essential to maintain skin health. Its anti-inflammatory properties can ameliorate irritation, redness, and itchiness. It can reduce inflammation in the skin cells, repair those cells, and help them regenerate. It moisturizes the skin and improves the skin barrier. With the proper amount of LNA, skin will look better and feel smoother. You may have noticed the mention of Omega 6 and Omega 3 Fatty Acids during the discussion of LA and LNA. Huh? Omegas? What are you talking about? I'm so glad you asked! I'm talking about a chemistry thing with fixed (or carrier) oils. It involves the location of the first double bond in the fatty acid molecule. I know, TMI, right? Well, yes and no. This is essential chemistry for those of us who are formulating products for others. For the purposes of this blog, I won't go into the chemistry, rather, I'll talk about two (of several) Omegas we need to watch for when we use fixed oils. You already know I'm talking about Omegas 3 and 6, and that the key Fatty Acids that have these designations are LNA and LA. Omega 6 FAs are pro-inflammatory while Omega 3s are anti-inflammatory, Just as too much Omega 6 can cause cause chronic inflammation and lead to a variety of inflammatory-based diseases (i.e. Alzheimer's, Type 2 Diabetes, etc), too much Omega 3 may lead to higher levels of LDL cholesterol, impair the immune system and white blood cell function, and cause bleeding. Consequently, it's important to keep these two Fatty Acids balanced. Currently, 3 parts Omega 6 to 1 part Omega 3 is considered optimal. Yes, a 3 to 1 ratio is correct. (I've seen other blogs erroneously say differently, but checked with my course professors to verify the correct ratio.) At most, a 5 to 1 ratio is considered to be within acceptable levels. In the west, the average person typically ingests a 16 to 1 (or higher) ratio. Is it any wonder the incidence of Diabetes, Heart Disease, High Cholesterol, and a host of other inflammatory diseases have become so prevalent? This is why nutritionists may recommend using Olive Oil or Canola Oil - they have that approximate 3 to 1 balance of Omega 6 to Omega 3. Peanut Oil, on the other hand, has about 33% Omega 6 but no Omega 3. It may add great flavor to food, but needs a counterbalance (i.e. salmon) that is rich in Omega-3 FAs. Hemp Seed Oil also has the "perfect balance" of Omega 6 to Omega 3, but it can't tolerate heat. So Hemp Seed Oil is good for oil and vinegar dressings, and it's great to use topically. Is it possible to have too little Omega-3 in our bodies? Yes. What happens if we don't have enough Omega-3? Are there signs or symptoms? Difficulties with vision, feeling weak, leg pain and/or difficulties walking, high cholesterol, lots of inflammation, and skin that feels scaly are all caused by, and may be symptoms of, a deficiency in Omega-3 Alpha-Linolenic Acid. The final take away from this is to educate yourself on what your body truly needs nutritionally. It may take some time to find the information you need, but you'll feel better and be healthier in the long run. Resources: 1. Parker, Susan, The Power of the Seed, Process Media, Port Townsend, Washington, ©2014 pages 58 - 64, 78 - 79, 245, 2. Foundation for Diet and Health, Alpha-Linolenic acid; ALA; 18:3 omega 3, https://www.diet-health.info/en/recipes/nutrients/nu/mx220-alpha-linolenic-acid-ala-183-omega-3 Accessed May 27, 2019 3. WebMD, Alpha-Linolenic Acid, © 2005 - 2019 WebMD LLC., https://www.webmd.com/vitamins/ai/ingredientmono-1035/alpha-linolenic-acid, Accessed May 27, 2019 4. NutrientsReview.com, Alpha-Linolenic Acid (ALA), NutrientsReview 2016, http://www.nutrientsreview.com/lipids/alpha-linolenic-acid-ala.html Accessed May 27 - 28, 2019 5. Quach, Helen, 20 Amazing Health Benefits of ALA (Alpha-Linolenic Acid), Selfhacked, Last updated February 20, 2019, https://selfhacked.com/blog/alpha-linolenic-acid/ Accessed May 27-28, 2019 6. the conscious life, Anti-Inflammatory Diet: How to Balance Omega-3 and Omega-6 Fatty Acids, 2009 - 2019, https://theconsciouslife.com/anti-inflammatory-diet-how-to-balance-omega-3-omega-6-fats.htm, Accessed May 28, 2019 7. Guyenet, Stephen, US Omega-6 and Omega-3 Fat Consumption over the Last Century, Whole Health Source: Nutrition and Health Science, April 10, 2011, https://wholehealthsource.blogspot.com/2011/04/us-omega-6-and-omega-3-fat-consumption.html, Accessed May 28, 2019 8. Simopoulos, A.P., Evolutionary aspects of diet, the omega-6/omega-3 ratio and genetic variation: nutritional implications for chronic diseases, Biomedicine & Pharmacotherapy, Volume 60, Issue 9, November 2006, pp 502 - 507 Science Direct, https://www.sciencedirect.com/science/article/abs/pii/S0753332206002435 Accessed May 28, 2019 We've learned what acute and chronic inflammation are, what causes them, and how they affect the body. Now, its time to discuss natural ways to relieve acute inflammation and to help reduce chronic inflammation.
We'll start with acute inflammation. RICE - Rest, ice, compression, elevation, and NSAIDS are considered by many to be the standard in treating an injury with inflammation, but others say, "wait, ice and NSAIDS don't help, and may harm". It's been interesting reading about the controversies dealing with the ice and NSAIDS steps. In a nutshell, the studies that have been done don't conclusively prove icing to be beneficial or harmful. It's the same with NSAIDS, but these medications carry the risk of other harmful effects on the body. What I suggest is to definitely rest, elevate, and use compression on a fresh injury (i.e. a sprained ankle). If you want to ice it, do so - it will probably help reduce pain and a little of the swelling. If you have no desire to ice it, then don't. Your body knows what it needs and your brain gets the signal to make that need sound, smell, or feel really good to you. In my personal experience, following many surgeries, I wanted to use ice and did so for several days post-op. I've also had many surgeries when the opposite was the case, and I didn't want ice and didn't use any at all. I recovered just fine in each case - my body knew what I needed and my brain signaled me to want or not want it. When it comes to NSAIDS, I have a more difficult time being unbiased. My body does NOT like NSAIDS at all -- I get severe stomach pain from them. I've also learned about some of the risks they pose to the body, so I won't recommend them. Are there things we can do in addition to RICE? Yes! There are herbs and carrier oils we can use both internally and externally, and essential oils we can use externally to help relieve pain and to promote the body to heal itself naturally. The beauty of the herbs, carrier oils, and essential oils is that they can be used for both acute and chronic inflammation. A wide range of herbs have scientifically-proven, significant anti-inflammatory properties. Included in this list are Ginger, Garlic, Oregano, Turmeric, Black Pepper, Rosemary, Lavender, Peppermint, Arnica, Calendula, St. John's Wort, Comfrey, Plantain, Plai, Galangal, Amla, Frankincense, Star Anise, and many more. Quite a few of these can be purchased at your local grocery store and incorporated into the foods you eat or used to flavor your coffee. Several can also be infused in water to use as compresses on an injured area or to drink as a tea. You can make tinctures by infusing them in a grain alcohol, then take a few drops of the tincture daily. When ingesting herbs, check to make sure it's safe. Some should only be used topically. If you are pregnant, breastfeeding, taking certain medications, are heading into surgery, or have chronic health conditions, certain herbs will be contraindicated. Fixed oils can be used in cooking, infused with herbs, and can serve as carriers to properly dilute essential oils. When cooking with these oils, it's important to get the proper balance of Omega 3 (Alpha-Linolenic Acid) to Omega 6 (Linoleic Acid) Essential Fatty Acids. That balance should be about a 1 to 3 ratio in order to maintain balance in the body's inflammatory process. For example, Olive Oil is comprised of 5% Alpha-Linolenic Acid and 5 - 15% Linoleic Acid. This is a great balance and the reason that Olive Oil is considered to be a healthy oil to use in cooking. A few other oils with the proper balance of Omega 3 to Omega 6 are Avocado Oil, Canola Oil, Sea Buckthorn Fruit Oil, and Walnut Oil. (Next week's blog will discuss these EFAs in more detail.) Fixed oils can also be infused with herbs and used topically or in cooking. The oils have their own therapeutic properties which can be enhanced with herbs. Trauma Oil is an herbally-infused oil. It's made from herbs that have been individually soaked in fixed oils for several weeks, then strained, then combined. Doing this allows the therapeutic properties of the herbs to transfer into the oils. The final oil can then be massaged into the skin to soothe localized pain and inflammation. Likewise, fixed oils serve as carriers for essential oils -- they 'carry' the essential oils into the skin. When you incorporate essential oils into combinations of fixed oils like Hemp Seed Oil, Tamanu Oil, Trauma Oil, Andiroba Oil, etc. you get an effective mix of anti-inflammatory and analgesic properties. Stronger blends can be made for short-term use during acute inflammation, and more diluted blends used for long-term, chronic inflammation. The list of essential oils that are analgesic and anti-inflammatory is too large for this blog, but here are a few of my favorites: Helichrysum, Copaiba, Ginger, Black Pepper, Turmeric, Geranium, Hops, Frankincense, Lavender, Peppermint, and Rosemary. Combinations of these oils can be used to help relieve both acute and chronic inflammation. An example of this is a blend I made to use after my last three surgeries. I added Copaiba Langsdorfii, Lavender, and Frankincense essential oils to Meadowfoam Oil and Jojoba that was infused with Comfrey Root and Calendula. All of these oils and herbs are safe to use during the two week post-op period and all have significant anti-inflammatory and analgesic properties. This blend helped keep the swelling under control, and while it did not eliminate all of my pain, it soothed it enough to make it bearable. There are a few final things to take note of here: 1. We don't want to immediately eliminate acute inflammation -- we need it to heal. The goal is to help the inflammatory process progress normally. 2. Chronic inflammation is what we do want to minimize or avoid. 3. There are steps we can take to reduce chronic inflammation. These steps include diet, exercise, lifestyle, and sleep, and can include the use of herbs, fixed oils, essential oils, and foods (which we haven't covered). 4. Most of us are not going to make sudden, drastic changes in our diets or lifestyle overnight. That's okay. Change just one thing at a time. Switch from using Peanut Oil to Olive Oil in your cooking or add ginger or peppermint to your morning cup of coffee. Once the 'new' action becomes routine, add another positive step. As you continue to repeat this process, eventually, you'll start feeling stronger, healthier, and more energetic -- oh, yeah, and your chronic inflammation will be reduced! We've learned how acute inflammation is the body's way of protecting and healing itself, and how chronic inflammation is an immune response that goes awry and may eventually lead to health issues as we age. This week, we'll discuss the link between inflammation and Alzheimer's Disease.
This topic is near and dear to my heart because my mother suffered from osteoarthritis (chronic inflammation) for much of her adult life. She went to college in her mid 40s and maintained a 4.0 gpa. Sometime in her 60s, she started forgetting things. This forgetfulness progressed until, eventually, she was diagnosed with Alzheimer's Disease. Watching her deteriorate mentally was one of the most heartbreaking things I've ever experienced. Mom passed away a little over a month ago, and I have to wonder how much her chronic inflammation contributed to her Alzheimer's, and if there were any steps that could have been taken to reduce the inflammation and prevent (or slow down) the progression of her Alzheimer's. I have a second reason for my concerns and my desire to find answers. I inherited my mother's arthritis -- it started when I was in my late teens -- so chronic inflammation has been a significant part of my life for several decades. I don't even want to imagine losing my mental faculties (my brain is my best feature). With an estimate of over 5 million people in the U.S. alone having Alzheimer's, this is personal to many of you as well. What is the link between inflammation and Alzheimer's? To answer this question, I'm going to quote sections from the research paper I wrote for my certification in Aromatherapy. This paper is titled: "The Role of Zingiber cassumunar Roxb (Plai) Essential Oil in Inflammation and Three Inflammatory Diseases" "The Role of Chronic Inflammation Inflammation is caused by the immune system responding to illness, injury, or damaged tissue. When cell damage occurs either by injury or invading pathogens, the body activates lymph and white blood cells to repair damage and restore the injured tissue. In acute situations, the swelling is temporary. Long term conditions, however, may cause chronic inflammation – even when there is no threat to the body. In this case, the white blood cells may begin to attack cells, tissues, and organs. Chemical imbalances and severe tissue damage may lead to chronic inflammation in one or more areas of the body. [27] When this happens, the body’s response can change from reparative to degenerative. As a result, chronic inflammation is believed to play a significant contributory role in in the cause and progression of arthritis, cancer, and Alzheimer’s disease. Nuclear-Factor-Kappa Beta, Cox enzymes, Interleukin-1β, MMP-13, and MMP-2, are all biological agents involved in the inflammatory process that can lead to arthritis, cancer, and Alzheimer’s disease." . . . "Nuclear Factor-Kappa Beta (NFkB) is a protein that senses damage in the body and sends signals to start and stop the inflammation process. As we get older, NFkB signaling increases and sets the body up for chronic inflammation, which causes greater vulnerability to diseases like Rheumatoid Arthritis, cancer, and Alzheimer’s disease. [11] Cox is an enzyme that the body produces during an inflammatory response. Its function is to produce prostanoids which are inflammatory hormones. While COX-1 is mostly good for the body and protects the digestive tract, COX-2 is a contributing factor to arthritis, cancer, and Alzheimer’s. [1, 9] Interleukin-1β (IL-1β) (a pro-inflammatory cytokine), MMP-13 (an enzyme), and MMP-2 (a gelatinase) are major factors in inflammation and cartilage destruction in Osteoarthritis. [24] " " Alzheimer’s Disease In Alzheimer’s disease, nerve cells and brain tissue are destroyed and the brain shrinks significantly over the course of several years causing a progressive loss of memory. In the end stages, the brain even loses the ability to signal the autonomic functions of breathing and pumping the heart. Swelling and oxidative stress cause and contribute to several biological processes in the body which lead to the destruction of brain tissue and Alzheimer’s Disease. [4] One of the neurologic processes affected by inflammation is with the neurotransmitters Acetylcholine and butyrycholine. These neurotransmitters carry signals from cell to cell in the brain – they allow thinking, talking, remembering, and functioning to take place. Acetylcholinesterase (AChE) and butyrycholinesterase (BChE) are enzymes that break down acetylcholine and butyrycholine respectively. Normally, AChE and BChE are balanced which keeps acetylcholine and butyrycholine balanced. However, chronic inflammation may interfere with AChE and BChE causing them to get out of balance, changing their roles from supportive to degenerative and negatively affecting the generation of neuronal cells. " "A second neurologic process influenced by inflammation is movement of Beta amyloid (β-A). β-A is a ‘sticky’ protein found in fatty membranes that surround nerve cells. Chronic inflammation may cause β-A to form clumps, or plaques. Small groups of these plaques (fibrils) may block cellular signaling at synapses which in turn, causes more inflammation by activating immune system cells. The immune cells come to try and fix the damage and eat the damaged nerve cells. [4] " "A third neurologic process affected by chronic inflammation is tau. Proteins in our bodies form a system of straight tracks to move nutrients and other important materials to different parts of the body. Tau is a protein that keeps those tracks straight. Neuro-inflammation can cause tau to collapse into twisted strands called tau tangles. In these areas, the transportation system falls apart and cells die. The cortex – especially the hippocampus – is eventually disintegrated in this process. [4] " As you can see, inflammation is a complicated process and has a significant effect on the brain. Chronic inflammation is not the sole factor in the development of Alzheimer's Disease, but it does play a key role. The good news is that we can take proactive steps to, hopefully, reduce both chronic inflammation and brain degeneration. Next week, we'll focus on some ways to deal with acute inflammation and reduce chronic inflammation naturally. Resources: 1. Dragoo, Karen "The Role of Zingiber cassumunar Roxb (Plai) Essential Oil in Inflammation and Three Inflammatory Diseases" 2017 Certification Research Paper for Aromahead Institute School of Essential Oil Studies Resources for my research paper: [1] All About COX2 - Selfhacked. (2017). Selfhacked. Retrieved 5 December 2017, from https://selfhacked.com/blog/cox2-natural-cox2-inhibitors/ [2] Anasamy, T., Abdul, A., Sukari, M., Abdelwahab, S., Mohan, S., & Kamalidehghan, B. et al. (2013). A Phenylbutenoid Dimer,cis-3-(3′,4′-Dimethoxyphenyl)-4-[(E)-3′′′,4′′′Dimethoxystyryl] Cyclohex-1-ene, Exhibits Apoptogenic Properties in T-Acute Lymphoblastic Leukemia Cells via Induction of p53-Independent Mitochondrial Signalling Pathway. Evidence-Based Complementary And Alternative Medicine, 2013, 114. http://dx.doi.org/10.1155/2013/939810 [3] Bhuiyan, M., Chowdhury, J., & Begum, J. (2008). Volatile constituents of essential oils isolated from leaf and rhizome of Zingiber cassumunar Roxb. Bangladesh Journal Of Pharmacology, 3(2), 69-73. http://dx.doi.org/10.3329/bjp.v3i2.844 [4] Brain Tour. (2011). Alz.org/braintour. Retrieved 6 December 2017, from https://alz.org/alzheimers_disease_4719.asp [5] Butje, A. (2010). Loving Terpinen-4-ol. Blog.aromahead.com. Retrieved 5 December 2017, from https://blog.aromahead.com/2010/08/12/loving-terpinen-4-ol [6] Danovi, S. (2017). Feeling the heat – the link between inflammation and cancer. Cancer Research UK - Science blog. Retrieved 5 December 2017, from http://scienceblog.cancerresearchuk.org/2013/02/01/feeling-the-heat-the-link-betweeninflammation-and-cancer/ [7] Deadly NSAIDS | American Nutrition Association. (2017). Americannutritionassociation.org. Retrieved 5 December 2017, from http://americannutritionassociation.org/newsletter/deadly-nsaids [8] Ethnobotany, Phytochemistry and Pharmacology of Zingiber cassumunar Roxb. (Zingiberaceae). (2015). Phytojournal.com. Retrieved 6 December 2017, from http://www.phytojournal.com/archives/2015/vol4issue1/PartA/3.1-921.pdf [9] Eustice, C. (2017). What Are the Drawbacks of Cyclooxygenase?. Verywell. Retrieved 5 December 2017, from https://www.verywell.com/cyclooxygenase-cox-1-and-cox-22552188 [10] Formulation Development of Plai Nanoemulsion Based on the Influence of Surfactant Combinations. (2012). Journal of the Science Faculty of Chiang Mai University. Retrieved 6 December 2017, from http://epg.science.cmu.ac.th/ejournal/journalDetail.php?journal_id=4558 [11] Goepp, J. (2017). What Is Nuclear Factor-Kappa Beta? - page 1 | Life Extension. LifeExtension.com. Retrieved 5 December 2017, from http://www.lifeextension.com/magazine/2006/7/report_nuclear/page-01 [12] Hauser, R. (2010). The Acceleration of Articular Cartilage Degeneration in Osteoarthritis by Nonsteroidal Anti-inflammatory Drugs. Journalofprolotherapy.com. Retrieved 5 December 2017, from http://www.journalofprolotherapy.com/pdfs/issue_05/issue_05_10_nsaids.pdf [13] Jalaja, M., Krishnakumar, K., Dineshkumar, B., Anish, J., David, P., & Joseph, C. (2013). Herbs for Alzheimer disease - A Review. Urpjournals.com. Retrieved 5 December 2017, from http://www.urpjournals.com/tocjnls/42_13v3i3_2.pdf [14] Kaewchoothong, A., Tewtrakul, S., & Panichayupakaranant, P. (2012). Inhibitory Effect of Phenylbutanoid-richZingiber cassumunarExtracts on Nitric Oxide Production by Murine Macrophage-like RAW264.7 Cells. Phytotherapy Research, 26(12), 1789-1792. http://dx.doi.org/10.1002/ptr.4661 [15] Koontongkaew, S., Poachanukoon, O., Sireeratawong, S., Dechatiwongse Na Ayudhya, T., Khonsung, P., & Jaijoy, K. et al. (2014). Safety Evaluation ofZingiber cassumunarRoxb. Rhizome Extract: Acute and Chronic Toxicity Studies in Rats. International Scholarly Research Notices, 2014, 1-14. http://dx.doi.org/10.1155/2014/632608 [16] Leelarungrayub, J., Manorsoi, J., & Manorsoi, A. (2017). Anti-inflammatory activity of niosomes entrapped with Plai oil (<em>Zingiber cassumunar</em> Roxb.) by therapeutic ultrasound in a rat model. International Journal Of Nanomedicine, Volume 12, 2469-2476. http://dx.doi.org/10.2147/ijn.s129131 [17] Li, X., Cai, X., Fan, F., Niu, H., Li, S., & Li, D. et al. (2015). Observation of sGAG content of human hip joint cartilage in different old age groups based on EPIC micro-CT. Connective Tissue Research, 56(2), 99-105. http://dx.doi.org/10.3109/03008207.2015.1009052 [18] Manosroi, J., Dhumtanom, P., & Manosroi, A. (2006). Anti-proliferative activity of essential oil extracted from Thai medicinal plants on KB and P388 cell lines. Cancer Letters, 235(1), 114-120. http://dx.doi.org/10.1016/j.canlet.2005.04.021 [19] Metcalfe, M., & Figueiredo-Pereira, M. (2010). Relationship Between Tau Pathology and Neuroinflammation in Alzheimer's Disease. Mount Sinai Journal Of Medicine: A Journal Of Translational And Personalized Medicine, 77(1), 50-58. http://dx.doi.org/10.1002/msj.20163 [20] Mortimer, S. (2009). Plai - a natural anti-inflammatory. Balance-holistics.blogspot.com. Retrieved 5 December 2017, from http://balance-holistics.blogspot.com/search?q=plai [21] Okonogi. (2012). Enhancement of anti-cholinesterase activity of Zingiber cassumunar essential oil using a microemulsion technique. Drug Discoveries & Therapeutics, 6(5), 249-255. http://dx.doi.org/10.5582/ddt.2012.v6.5.249 [22] Panthong, A., Kanjanapothi, D., Niwatananant, W., Tuntiwachwuttikul, P., & Reutrakul, V. (1997). Anti-inflammatory activity of compound D {(E)-4-(3′,4′dimethoxyphenyl)but-3-en-2-ol} isolated from Zingiber cassumunar Roxb. Phytomedicine, 4(3), 207-212. http://dx.doi.org/10.1016/s0944-7113(97)80069-4 [23] Rakoff-Nahoum, S. (2007). Cancer Issue: Why Cancer and Inflammation?. PubMed Central (PMC). Retrieved 5 December 2017, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1994795/ [24] Rujirek, C., Siriwan, O., Siriwan, T., Prachya, K., Ampai, P., & Vichai, R. (2012). Chondroprotective potential of bioactive compounds of Zingiber cassumunar Roxb. against cytokine-induced cartilage degradation in explant culture. Journal Of Medicinal Plants Research, 6(39), 5204-5213. http://dx.doi.org/10.5897/jmpr11.1633 [25] Shacter, E., & Weitzman, S. (2002). Chronic Inflammation and Cancer | Cancer Network | The Oncology Journal. Cancernetwork.com. Retrieved 5 December 2017, from http://www.cancernetwork.com/colorectal-cancer/chronic-inflammation-and-cancer [26] Singh, D., Gupta, M., Kesharwani, R., & Misra, K. (2013). Comparative docking and ADMET study of some curcumin derivatives and herbal congeners targeting β-amyloid. Network Modeling Analysis In Health Informatics And Bioinformatics, 2(1), 13-27. http://dx.doi.org/10.1007/s13721-012-0021-7 [27] Szalay, J. (2015). Inflammation: Causes, Symptoms & Anti-Inflammatory Diet. Live Science. Retrieved 6 December 2017, from https://www.livescience.com/52344inflammation.html [28] ToxTutor - Systemic Toxic Effects. (2017). Toxtutor.nlm.nih.gov. Retrieved 6 December 2017, from https://toxtutor.nlm.nih.gov/03-003.html [29] Udomlak, S., Prapassorn, R., Putthita, P., Sopida, C., & Vichien, K. (2009). Chemical Composition and Physical Properties of Oil from Plai (Zingiber cassumunar Roxb.) Obtained by Hydro Distillation and Hexane Extraction. Kasetsartjournal.ku.ac.th. Retrieved 5 December 2017, from http://kasetsartjournal.ku.ac.th/kuj_files/2010/A1003081306505000.pdf [30] Viscosupplementation, H. (2017). Hyaluronic Acid / Viscosupplementation | Patient Education. Patient Education. Retrieved 5 December 2017, from https://cartilage.org/patient/about-cartilage/can-i-be-treated-without-surgery/hyaluronicacidviscosupplementation/ Recommended Reading/Websites: https://alz.org/alzheimers-dementia/what-is-alzheimers/brain_tour https://www.alzdiscovery.org/news-room/blog/inflammation-the-driver-of-alzheimers-disease https://www.news-medical.net/health/Inflammation-and-Alzheimers-Disease.aspx https://thevaccinereaction.org/2017/11/chronic-inflammation-in-alzheimers-disease/ https://sanescohealth.com/alzheimers-disease-and-inflammation/ https://bodyecology.com/articles/alzheimers-and-inflammation/ As we saw last week, acute inflammation is the body's natural immune reaction to heal injuries, combat pathogens, and to protect itself. This week, we'll look at what chronic inflammation is, some of its causes, and how it affects the body.
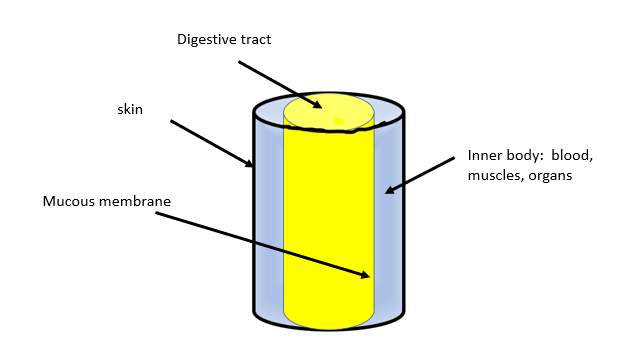
Chronic inflammation means swelling that continues for an extended period of time. Tendonitis is an example of chronic inflammation. A tendon attaches muscle to bone. Overuse with repetitive motion, or injury like a strain or tear, can cause the tendon to swell. When that swelling persists (even though the injury itself has healed), the doctor may diagnose tendonitis. In such a case, the swelling may not be outwardly visible, but there is heat, pain, and limited range of motion. The example above tells us that overuse of a body part can be one cause of chronic inflammation. There are several more potential causes -- some that are understood, some partially understood, and some that have not yet been discovered. Genetics, aging, injury, infection, auto-immune disease, exposure to chemicals/pollution, smoking, poor diet, obesity, excessive use of alcohol, and chronic stress can all be contributing factors to and/or direct causes of chronic inflammation. However, two people could experience the exact same contributing factors, but only one of them develops chronic inflammation. Scientists are still trying to understand how and why that happens. What we do know more about is the effect chronic inflammation has on the body. Because chronic inflammation can last for years, it can harm rather than heal the body. If it's in one or more joints, it can cause further damage to soft tissue (i.e. cartilage). Inflammation that continues for many years, will eventually cause cell damage, scarring, and possibly DNA damage. If left unchecked, it can cause diseases like diabetes, asthma, heart disease, OA, RA, atherosclerosis, some types of cancer, autoimmune diseases, Crohn's, UC, Psoriasis, Nephritis, Myalgias, MS, FM, Colitis, and neurodegenerative diseases (example: Alzheimer's Disease). Many of these diseases then cause more inflammation, and the cycle starts to spiral out of control. The list goes on, but you're starting to see that chronic inflammation plays a role in the development of many of the diseases we encounter as we age. This list looks scary -- and it is. The good news is that there are steps we can take to reduce chronic inflammation and hopefully, avoid its ravages on our bodies. We'll look at these steps in two weeks. Before that, I want to show in more detail exactly how chronic inflammation impacts our bodies. So, next week, I'm going to focus on one of the above diseases from the list - Alzheimer's Disease - and show how chronic inflammation is a key contributing factor in the onset and continuing degeneration of the brain. Resources: 1. PPT Health, Diseases Caused by Chronic Inflammation, 2019, https://www.ppt-health.com/inflammation-relief/diseases-caused-by-chronic-inflammation/, Accessed May 5 - 7, 2019 2. Santos-Longhurst, Adrienne, Understanding and Managing Chronic Inflammation, Healthline, July 27, 2018, https://www.healthline.com/health/chronic-inflammation, Accessed May 5 - 7, 2019 3. Nordqvist, Christian, Everything you need to know about inflammation, Medical News Today, Last updated Nov. 24, 2017, https://www.medicalnewstoday.com/articles/248423.php, Accessed May 5 - 7, 2019 Inflammation plays a huge role in our lives - from injuries/illnesses to chronic inflammation to auto-immune diseases. Learning when and how to control inflammation can help us live happier, healthier lives. I'm writing a 4 part series to describe the process and impact of inflammation. Part 1 of this series will explain how inflammation is a part of the immune system response to repair damage to the body and to fight off pathogens. Part 2 will discuss what chronic inflammation is, what causes it, and how it impacts the body. Part 3 will detail how chronic inflammation affects the brain. Part 4 will illuminate some things we can do naturally to help inflammation heal acute situations and to (hopefully) reduce chronic inflammation. Part 1: Inflammation as a Part of the Immune System Response If you sprain your ankle or get a cut, you experience swelling, heat, bruising or redness, and pain. In other words, your immune system is sending extra blood and immune cells to the area to 'fix' the injury. Let's look at how the whole process works. Your immune system is comprised of several parts that are designed to protect and repair your body. The first parts are barriers - cells, skin, organs, cilia, mucous membranes, and urine/waste that are designed to keep pathogens (invaders) out. Your skin is the first organ that protects you - it keeps your innards on the inside and everything else outside. Hair in the nose and ears help trap dust and irritants to prevent them from entering the body. Cilia in the lungs help move invaders back out of the lungs. Mucous membranes cover the respiratory, digestive, and reproductive tracts. These areas are inside our bodies, but they still provide a barrier between the external and the internal. To help you understand this, I've drawn a very simplistic diagram below. Obviously, this cylinder isn't a body, but it lets us easily visualize the outer skin (the thick black lines), the digestive tract (the yellow, inner cylinder), the mucous membrane (the thin black lines), and the inner body (the blue part). In a sense, even though the digestive tract is inside our bodies, it's still part of the external skin (but mucusy). Finally, foreign objects and pathogens that we ingest and that our bodies can't use for nutrition, continue on through the digestive tract until they are eliminated through urine/waste. These barriers are a part of the immune system and are maintained by other parts of the immune system.
What happens then if part of the barrier gets broken (i.e. you get a cut)? This is where lymph cells and fluids and white blood cells (WBCs) come into play. They immediately go to work signaling the body to send blood, plasma, and other immune cells (more lymph and WBCs) to rush to the area to fight off any pathogens (invaders) that have entered through the cut and to start repairing the skin. The extra blood causes redness and heat, and the extra plasma and lymph causes swelling and pain (which is in addition to the pain caused by damaged nerve cells). With the swelling and pain, you may not be able to use the injured area normally. This type of inflammation is called 'Acute Inflammation' and it's healthy - it's good for us. It's temporary, and will resolve as it helps the body heal the injury. If our immune systems fight off pathogens, then why do we get sick? Sometimes a pathogen multiplies faster than our immune system can figure out how to kill it. Imagine you breathe in some flu germs. If it's your first exposure to these germs, many types of cells in your body send out a message to lymphocytes (soldier cells) to come quick and fight the pathogen. These lymphocytes rush to the area and start fighting the (rapidly multiplying) flu cells. If the lymphocytes win quickly, you may not even know the pathogen was there. However, if the lymphocytes take a while to figure out how to kill the flu cells, you'll start to feel symptoms - heat in the form of fever (which also kills the pathogen), weakness because your body is using all its energy to defeat the pathogen, mucus full of the dead pathogen and immune cells that were killed in the fight, and so on. If your sinuses are the 'battleground', you'll experience swelling from all the extra lymph that's been sent into battle. As pathogen cells and lymphocytes die in the battle, you'll experience extra mucus - your body's way of expelling the dead cells. Again, this is acute inflammation because it's sudden, severe, and short term. It's good inflammation - it means your body is working the way it's supposed to. So, acute inflammation is a part of the body's natural defense to injury or invasion. We need acute inflammation to set the healing process in motion, to eliminate dead and damaged cells, and to get rid of pathogens. Unfortunately, not all inflammation is good for us. When we find ourselves under long-term, high-level stress, the inflammatory process may become chronic. When that happens, it can have a serious impact on our overall health. Next week's blog will discuss what chronic inflammation is, some of its causes, and some of the ways it significantly affects our bodies. Resources: 1. . Aromahead Institute, School of Essential Oil Studies, A&P Course, www.aromahead.com 2. Hooper, Cameron, Everything You Need to Know About Inflammation; Naturalife; April 6. 2017; https://naturalife.org/health/everything-need-know-inflammation, ,Accessed April 30, 2019 3. Reference*, How Does the Immune System Work With Other Body Systems?, https://www.reference.com/science/immune-system-work-other-body-systems-2adf1bf181240c39, Accessed April 30, 2019 4. Reviewed by Yamini Durani, MD, Immune System, KidsHealth from Nemours, May 2015, https://kidshealth.org/en/parents/immune.html, Accessed April 30, 2019 We've been looking at what fixed and essential oils are, and we've charted their differences. Looking at the chart, we see that carrier (fixed) oils can be used on the skin without diluting and are used to dilute essential oils for topical use. Today, we'll discuss some of the factors we take into consideration when blending carrier and essential oils.
The first factor to take into consideration is the purpose of the blend. Are you trying to make a blend that will keep the skin healthy and glowing? If blending for oily, acne-prone skin, carriers like Sacha Inchi, Jojoba, Black Seed (Nigella), and/or Kukui could be combined with Tea Tree, Lavender, Cedarwood, and/or Petitgrain essential oils. A blend for mature, dry skin, on the other hand, might include carrier oils like Avocado, Macadamia Nut, and/or Marula with Carrot Seed, Frankincense, Lavender, and/or Rose essential oils. All of these oils are skin nourishing/healing, but the type of skin determines the choice of oils. Are you trying to make a blend to soothe achy joints? A combination of Castor Oil, Hemp Seed Oil, and Tamanu Oil could be mixed with Plai, Helichrysum italicum, and Copaiba essential oils. Castor Oil will help the blend absorb deep into the tissues of the body. All three carriers have anti-inflammatory and analgesic properties as do the essential oils. The second factor we look at is the person who'll be using the blend - his/her age, skin type, potential allergies, health issues, medications, and constitution. Once we know the purpose of a blend, we need to find out about the person who'll use it in order to choose the best oils for his/her particular circumstance. If the person has oily, acne-prone skin, then oils high in Linoleic Acid, like Grapeseed or Evening Primrose are best. Someone with mature, dry skin would benefit from oils that are high in Oleic Acid such as Olive Oil or Macadamia Nut Oil. But what if the person with dry skin has a tree nut allergy? In such a case, oils made from tree nuts are contraindicated for any blend made for that person. Instead, we might choose Olive, Safflower, or Sesame Seed Oils. It's the same for allergies to specific plant families -- if we know the person has a specific plant allergy, we eliminate from consideration any oils -- carrier or essential -- that might come from that plant or plant family. If the person doesn't know what his/her allergies are, but tends to react to many topical products, the wisest course of action is to do 'patch tests' first. Age, medical conditions, and medications must also be taken into consideration when blending. Essential oil choices are affected in this case. Some examples: 1. Eucalyptus essential oil should not be used with a child under the age of 10. 2. Wintergreen essential oil is contraindicated for those with a blood-clotting disorder. 3. German Chamomile essential oil may interfere with certain medications, like some antidepressants. In cases like these, there are plenty of other essential oils to choose from which will have similar therapeutic properties and be safe for the recipient of the blend. Constitution is usually discussed in herbal circles rather than in aromatherapy; however, I'm including it here because I see an application for constitution with the oils as well. In herbalism, constitution involves the nature of a person -- whether (s)he is normally hot or cold, damp or dry -- and what his/her current condition is -- hot or cold, damp or dry. Like herbs, essential oils can be warming or cooling, and drying or moistening and carrier oils can be drying or moisturizing. The closest term to this in aromatherapy is 'Energetics', but the two terms are not completely synonymous. When blending for someone who is always cold and has dry skin, we would normally choose oils that are warming and moisturizing. But if that person is experiencing a 'hot' situation i.e. a sprained ankle that is swollen and warm to the touch, we would choose a cooling oil. In such a case, we might use Peppermint, Lavender, and Geranium essential oils with Hemp Seed and Tamanu carrier oils. In understanding this, we consider the person as a whole and blend to bring balance to the whole person. The third factor to take into consideration is the chemical composition of the oils. Both groups of oils consist of nature-made chemicals. Carriers have a handful of long-chain Fatty Acids, and each essential oil has, on average, about 100 different types of short-chain carbon/hydrogen molecules. You might want to make a blend that focuses on one or two EO chemicals for a specific therapeutic benefit. For example: a blend high in Beta-caryophyllene and Alpha-humulene would be great for immune support and chronic inflammation. In this case, Copaifera langsdorfii, L. could be combined with Hops essential oil. Choosing carrier oils with the optimal 3 : 1 (or 2 : 1) ratio of Omega 6 (pro-inflamatory) to Omega 3 (anti-inflammatory) Fatty Acids would add a great impact. (Yes, we do need more Omega 6 than Omega 3.) Hemp Seed, Kukui Nut, and Red Raspberry Seed oils are good choices here. [I'll write a series of blogs on inflammation soon.] Conversely, you may want to mix up chemicals with similar therapeutic properties. Let's say you want to make an antifungal blend. You might use essential oils high in camphor (like Rosemary ct. camphor), carotol (in Carrot Seed EO), alpha-bisabolol (in Balsam Popular), and citronallol (in Geranium). Adding those essential oils to a combination of Coconut and Hemp Seed carrier oils (both of which are also antifungal) could meet your needs. Since camphor is a Ketone, it would be harsh on the skin. That harshness is counterbalanced by the other chemicals (monoterpenols) and the carrier oils. The final factor we'll discuss in this blog is consistency and absorption rate of the carrier oils. If you are making a blend for massage, you'll want carriers that stay oily on the skin and are slow to absorb. Oils like Avocado Oil, Fractionated Coconut Oil, and Sweet Almond Oil fit that criteria. Essential oils used in massage would be determined by purpose -- perhaps you want oils that are uplifting and will help your muscles relax. Lavender, Roman Chamomile, and Frankincense would work well here. A blend to moisturize dry skin from frequent hand washing would need to absorb quickly. Jojoba, Macadamia Nut, and Safflower oils absorb very quickly. The hands feel dry (not greasy) after application. Adding Frankincense, Vetiver, and Myrrh or Patchouli and Sandalwood would add to the skin-healing effect. The above factors are all inter-related. Purpose, chemical composition, consistency and absorption, skin type, constitution, and health are all pieces of the whole picture when deciding on individual components of a personal blend. Aromatherapists are trained to look at these, and many more aspects, when they create blends. Understanding these oils in-depth requires education, which is why, if you're having someone blend for you, it's best to have a certified aromatherapist do it. Likewise, you can easily blend for yourself - just be sure to research each component thoroughly. P.S. Please feel free to ask me questions. I love to share what I've learned! |
Archives
February 2021
CategoriesAuthorKaren Dragoo |
 RSS Feed
RSS Feed