 Our immune systems are designed to "remember" pathogens and how to fight them after we encounter them for the first time. This 'memory' is why we become immune to certain diseases once we've had them or been vaccinated against them. Then, why do we catch certain illnesses multiple times? Likewise, why do we need to repeat some vaccinations? Unfortunately for us, some of these invaders survive by mutating. These mutations are the reason we can get the same illness over and over again. Let's take a more detailed look at how this works in regards to the flu. There are thousands of variations of flu viruses! These variations are broken down into four types - A, B, C, and D. Type A affects human beings and animals; types B and C affect humans only; and type D affects only cattle and pigs. Let's look at each type of human flu individually. We'll start with, type C, which causes only mild respiratory symptoms like stuffy nose, coughing, headache, congestion, etc. Scientists do not believe it's responsible for seasonal epidemics, and, because it tends to be rare and mild, flu vaccines are not designed to protect against it. Type B flu is usually mild, but can get severe. It is one of the strains responsible for seasonal epidemics and is included in flu vaccines. Type B flu is divided into two 'lineages' then into smaller groups and finally into subgroups. Type A is the most dangerous of the flu viruses. It affects humans and a variety of animals, and is responsible for both epidemics and pandemics (worldwide epidemics). This category of flu is divided into subtypes of both hemagglutinin and neuraminidase, which are surface proteins, and is further broken down into groups and subgroups. While there are nearly 200 possible subtype combinations for Type A flu, only two are seen on a regular basis - A(H1N1) and A(H3N2), and they are included in the annual flu vaccine. Because type A can jump from species to species, it has the potential to mutate much more drastically than types B or C. This is why type A is the only type of flu that creates pandemics. 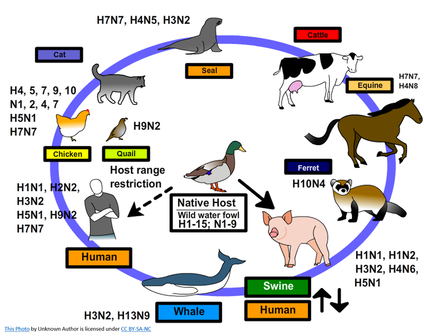 [A(H1N1) refers to Influenza Virus A hemagglutinin 1, neuraminidase 1. You might remember H1N1 from 2009 - it was referred to as 'Swine Flu'. This particular strain of flu started out infecting pigs. It mutated and jumped to humans. Since it had never infected humans before, it became pandemic fairly quickly because human immune systems had to learn how to defeat it. It's full designation is H1N1 pdm09. Interestingly, and tragically, the flu pandemic of 1918 was an avian version - also an H1N1 flu that jumped from birds to humans.] The thing about flu is that each new generation of viruses being produced in your epithelial cells has mutated from its parent virus because it has added small bits of your cellular genetic information to its own! Your immune system has to keep adapting to each new generation in order to effectively fight it. In addition, if you cough or sneeze near someone, the virus particles you spread to that person are slightly different from the virus particles that initially made you sick. If a mutation is similar enough to a strain you've had before or been vaccinated against, your immune system is likely able to recognize it and is better able to fight it before it can become severe. Larger mutations, on the other hand, (like the ones that jump species) create a greater chance of causing severe illness and spreading more widely. The constant mutations occurring among the various types of flu make it impossible for scientists to 'cure' the flu. The best they can do is look at historical patterns of infection and try to predict what next year's version(s) will be. The pharmaceutical companies create their vaccines based on these predictions. The vaccines contain weakened or dead virions from Types A(H1N1), A(H3N2), and one of the two Type B lineages. If they predict correctly, your Flu Vaccine helps you avoid the flu; however, if the prediction is wrong, or if the mutation(s) are too great, you may still catch it. We can take the information we now know about the flu and extend it to a virus that is causing new, global concern: Corona Virus. Next week's Monthly Tidbits blog will look at what scientists know about the new Corona Virus.
Resources: 1. Centers for Disease Control and Prevention; How the Flu Virus Can Change: “Drift” and “Shift”, U.S. Centers for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases (NCIRD), Page last reviewed: October 15, 2019, Accessed February 12, 2020, https://www.cdc.gov/flu/about/viruses/change.htm 2. Centers for Disease Control and Prevention; Influenza Virus Genome Sequencing and Genetic Characterization, U.S. Centers for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases (NCIRD), Page last reviewed: October 15, 2019, Accessed February 12, 2020, https://www.cdc.gov/flu/about/viruses/change.htm 3. Centers for Disease Control and Prevention; Types of Influenza Viruses, U.S. Centers for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases (NCIRD), Page last reviewed: November 18, 2019, Accessed February 12, 2020, https://www.cdc.gov/flu/about/viruses/change.htm 4. Butje, Andrea, Viruses and the Immune System: Influenza, Aroma Institute School of Essential Oil Studies, Accessed February 12, 2020, https://www.aromahead.com/online-course/viruses-and-the-immune-system/reference/general-reference/influenza 5. WebMD, Types of Flu, WebMD LLC. , © 2005 - 2020, Accessed February 12, 2020, https://www.webmd.com/cold-and-flu/advanced-reading-types-of-flu-viruses#1 6. Centers for Disease Control and Prevention; How Influenze (Flu) Vaccines are Made, U.S. Centers for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases (NCIRD), Page last reviewed: December 12, 2019, Accessed February 17, 2020, https://www.cdc.gov/flu/prevent/how-fluvaccine-made.htm 7. Ana Mosterín Höpping, Judith M. Fonville, Colin A. Russell, Sarah James, Derek J. Smith, Influenza B vaccine lineage selection—An optimized trivalent vaccine Vaccine. 2016 Mar 18; 34(13): 1617–1622. doi: 10.1016/j.vaccine.2016.01.042 PMCID: PMC4793086, Accessed February 17, 2020, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4793086/ Comments are closed.
|
Archives
February 2021
CategoriesAuthorKaren Dragoo |
 RSS Feed
RSS Feed